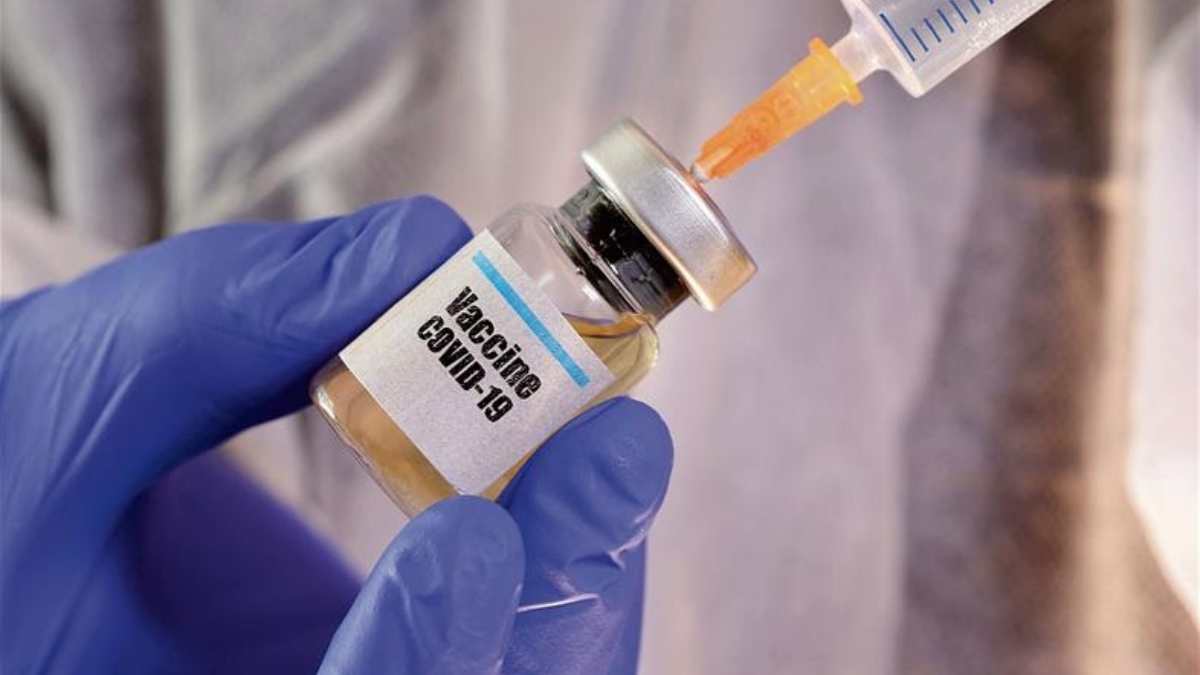
Among the vaccines against Covid-19 likely to become available in India in early 2021, Covaxin is an indigenous vaccine, being developed by Bharat Biotech International Limited (BBIL), Hyderabad, in collaboration with the Indian Council of Medical Research (ICMR), New Delhi. The candidate is an inactivated whole virion vaccine.
Most of the vaccine manufacturers based in Western countries are employing ‘smart’ and ‘sexy’ newer technologies to develop vaccines against the SARS CoV-2 virus: be it mRNA technology (Moderna and Pfizer/BioNTech) or genetically engineered adenoviruses (AstraZeneca/Oxford University and Russia’s Gamaleya Research Institute of Epidemiology and Microbiology). However, there are a few manufacturers, notably in India, China and Kazakhstan, which are pursuing an old, trusted and time-tested approach to make a vaccine against the new coronavirus – by using an inactivated/killed virus. First tried successfully in the 1930s, unlike the mRNA or the adenovirus carrier strategy, the inactivated approach has a solid track record. It has to its credit the development of vaccines for diseases like influenza, cholera, plague, rabies, hepatitis A, polio (IPV), etc. The vaccine efficacy of inactivated vaccines has traditionally been between 60% and 70%.
Also Read: We are at the doorstep of getting a coronavirus vaccine: Dr V.K. Paul
The approach of making an inactivated vaccine is remarkably simple. Isolate the virus from a sick/infected person, grow it in the lab, kill/inactivate it, purify, add an adjuvant, and the vaccine is ready! Its storage is also not a problem, as the temperature of a household refrigerator (+2 to +8°C) is all that is necessary. Refrigeration at sub-zero temperatures is not required.
When injected into humans, inactivated vaccines produce immunity. But because the virus is dead, they interact with the immune system differently. The immune response to live and newer vaccines is similar to encountering the virus itself, resulting in the development of humoral (antibodies) and cellular immunity (mediated by T lymphocytes). Inactivated vaccines produce antibodies but show little or no cellular immunity. Since killed or inactivated viruses can’t replicate, they tend to provide a shorter length of protection than live vaccines, and are more likely to require boosters to create long-term immunity. Adjuvants are added to trigger a strong immune response. However, adjuvants can cause more local reactions (such as redness, swelling, and pain at the injection site) and more systemic reactions (such as fever, chills and body aches) than non-adjuvanted vaccines. Traditionally, aluminium-based adjuvants like aluminium hydroxide or aluminium phosphate have been used to trigger strong humoral immunity but with little or no cellular immunity. Newer adjuvants are now available which help to elicit cellular response and make the protection stronger and longer.
The inactivated approach offers some distinct advantages though. The greatest one is that there is no risk of inducing the disease as the virus has been inactivated. The viruses can be rapidly grown in the lab and scaled up using well-established infrastructure and methods. There are very few safety concerns. Inactivated vaccines are easier to store and transport as normal refrigerator temperatures suffice. Because the whole virus is presented to the immune system, it is likely to target not only the spike protein of the SARS-CoV-2, but also the matrix, envelope and nucleoproteins. These vaccines therefore express a wide range of viral antigens. In general, two doses given with an interval of 14 days can give an antibody reaction in four weeks. On the downside, the inactivated vaccines produce mainly humoral immunity (antibodies), invariably require multiple doses, and often require an adjuvant. Correlates of protection afforded by inactivated vaccines are also not known as of now.
China produced the world’s earliest inactivated SARS CoV-2 candidate vaccines. Sinovac Life Sciences, Beijing developed CoronaVac, and the two branches of China National Biotec Group (CNBG) viz. Wuhan Institute of Biological Products and the Beijing Institute of Biological Products affiliated to the China National Pharmaceutical Group (Sinopharm) developed ‘SARS-CoV-2’ vaccine and ‘BBIBP-CorV’ vaccine, respectively. The Bharat Biotech’s vaccine appears to have an advantage over the Chinese vaccines in its composition. Instead of using the traditional aluminium hydroxide as an adjuvant, it is using an adjuvant called Toll Like Receptor 7/8 (TLR-7/8). This is known to enhance not only humoral but also cellular immune responses. The inactivated vaccine formulation containing TLR7/8 agonist adjuvant was used in preclinical/animal studies in Hyderabad. It has shown to induce Th1 biased antibody responses with elevated IgG2a/IgG1 ratio and increased levels of SARS-CoV-2 specific IFN-γ+ CD4 T lymphocyte response.
It is not known whether the Haryana minister received the placebo or the vaccine, since it is a double-blind trial. Even if he received the candidate vaccine, he got only the first dose. The trial vaccine can offer protection only two weeks after the second dose.
The writer is former head of the Epidemiology & Communicable Diseases Division of the Indian Council of Medical Research (ICMR).