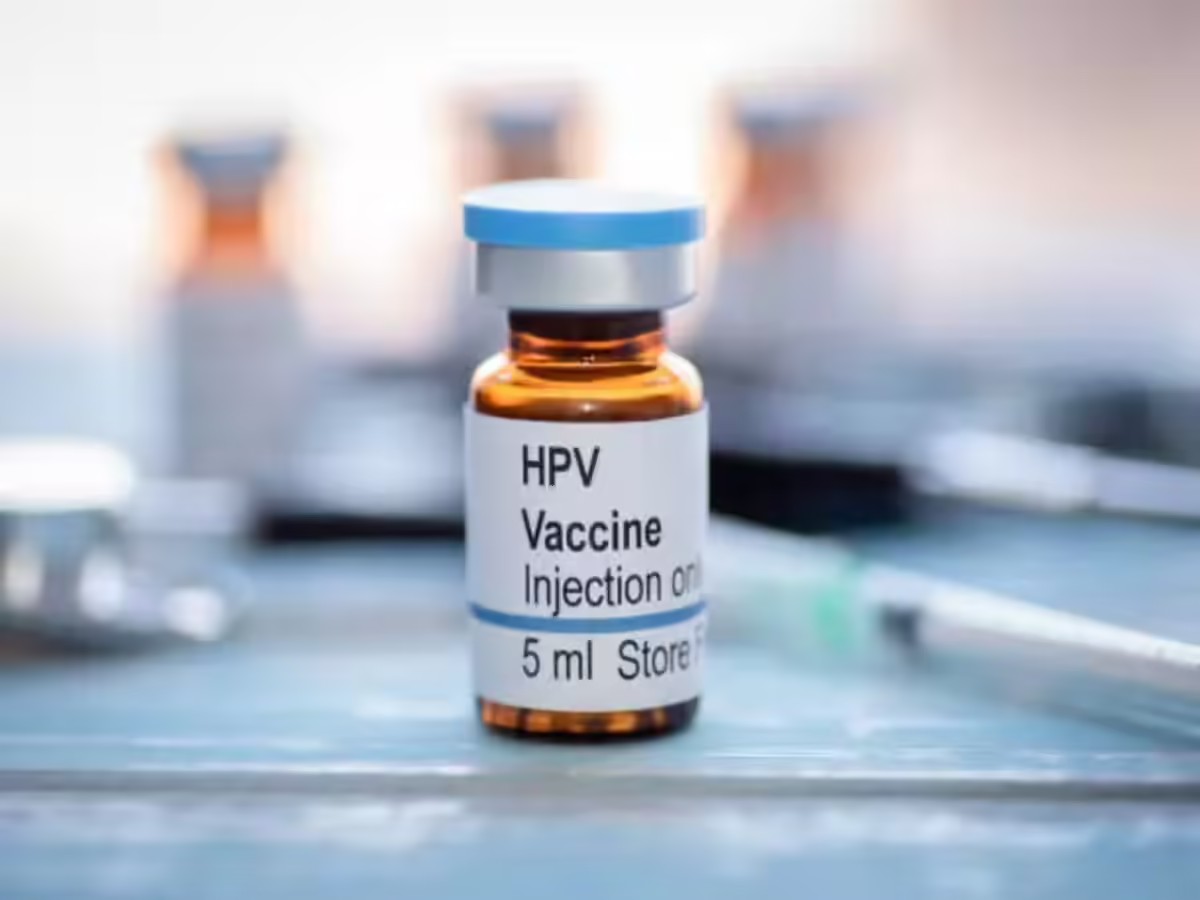
NEW DELHI: In a major step towards strengthening women’s health and preventing avoidable cancers, the Government of India is set to launch a nationwide Human Papillomavirus (HPV) vaccination campaign targeting 14-year-old girls. The special drive, which will be conducted under the Universal Immunisation Programme (UIP), marks a significant move in the country’s efforts to reduce the burden of cervical cancer.
Cervical cancer remains the second most common cancer among women in India, with nearly 80,000 new cases and over 42,000 deaths reported annually. Scientific evidence shows that almost all cases are caused by persistent infection with high-risk HPV types, particularly HPV 16 and 18, which account for more than 80 per cent of cases in the country. Despite being largely preventable through vaccination and early screening, the disease continues to claim thousands of lives each year.
The forthcoming campaign seeks to address this gap through early prevention. By targeting girls at the age of 14—well before potential exposure to the virus—the programme aims to provide long-term protection and significantly lower future incidence rates of cervical cancer.
India will use Gardasil, a quadrivalent HPV vaccine that protects against HPV types 16 and 18, responsible for cervical cancer, as well as types 6 and 11. The vaccine has been extensively studied worldwide and has
demonstrated high efficacy in preventing cervical cancer caused by vaccine-covered HPV types. More than 500 million doses have been administered globally since its introduction in 2006, with a strong safety record. Evidence reviewed in recent years indicates that a single-dose schedule offers protection comparable to two-dose regimens for the recommended age group.
In June 2022, the World Health Organization’s Strategic Advisory Group of Experts on Immunization (SAGE) evaluated emerging data and concluded that a single-dose HPV vaccine provides protection comparable to two-dose schedules. Subsequently, the WHO Position Paper on HPV Vaccine, issued in December 2022, stated that a single-dose schedule may be used as an off-label option in girls and boys aged 9-20 years, noting comparable efficacy and duration of protection. However, it recommends at least two doses—and where feasible, three—for individuals who are immunocompromised or living with HIV.
With the rollout, India will join more than 160 countries that have already introduced HPV vaccination into their national schedules, and over 40 countries implementing single-dose schedules to improve coverage and affordability.
Vaccination will be voluntary and provided free of cost at designated government health facilities, including Ayushman Arogya Mandirs (Primary Health Centres), Community Health Centres, Sub-District and District Hospitals, and Government Medical Colleges. Each session will be conducted under the supervision of trained Medical Officers, with arrangements in place for post-vaccination observation and management of rare adverse events. All sites will be linked to 24×7 government facilities to ensure immediate medical support.
Vaccine procurement has been secured through a transparent mechanism, with supplies made available under India’s partnership with Gavi, the Vaccine Alliance. The vaccines meet stringent regulatory and cold-chain standards and will be distributed across all States and Union Territories.
The government has urged parents and guardians to ensure that their 14-year-old daughters receive the HPV vaccine once the campaign begins, describing vaccination as a critical preventive step that can save lives and secure a healthier future for India’s young women.